Gall bladder stones are a common yet painful condition that can cause a variety of symptoms, from mild discomfort to severe pain. When it comes to treatment, surgery is often recommended if the condition worsens. At
Dr Gastro, we specialize in
Gall Bladder Stone Surgery in Ahmedabad, offering the latest surgical methods to ensure a quick and efficient recovery. But when is the right time to consider surgery? Let’s explore the signs, causes, and the best treatment options for gall bladder stones.
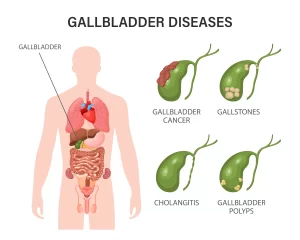
What Are Gall Bladder Stones?
Gall bladder stones (also known as
cholelithiasis) are hardened deposits of bile that form in the gall bladder. The gall bladder, a small organ located just beneath the liver, stores bile, which helps digest fats. These stones can vary in size and may be composed of cholesterol or bilirubin.
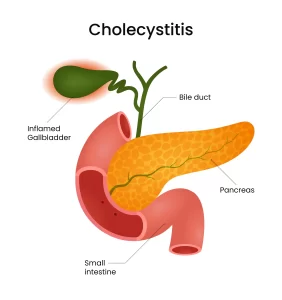
Gall bladder stones may not cause immediate symptoms, but they can lead to painful complications if left untreated. In some cases, they can block the bile ducts, leading to a condition called
cholecystitis or even jaundice, which is why it’s important to understand when surgery might be necessary.
Symptoms of Gall Bladder Stones: When Should You Seek Treatment?
Some people with gall bladder stones may not experience symptoms. However, if you’re dealing with any of the following, it might be time to consider
gall bladder stone surgery in Ahmedabad:
- Abdominal Pain: Often severe, this pain typically occurs in the upper right side of the abdomen and may last for several hours. It’s usually triggered after eating a fatty meal.
- Indigestion and Bloating: Feeling full, bloated, or having indigestion after meals can be signs of gall stones.
- Nausea or Vomiting: Persistent nausea and vomiting, particularly after eating, are common symptoms.
- Jaundice: Yellowing of the skin or eyes can occur if a gall bladder stone blocks a bile duct.
- Fever and Chills: If an infection is present, fever may develop, which requires immediate medical attention.
If you experience any of these symptoms, it’s best to consult a specialist for a diagnosis.
 When Is the Right Time for Gall Bladder Stone Surgery?
When Is the Right Time for Gall Bladder Stone Surgery?
The decision to have
gall bladder stone surgery depends on several factors. Here are the key signs that surgery may be necessary:
- Frequent or Severe Pain
If you experience recurrent episodes of intense abdominal pain (biliary colic) due to gall stones, surgery might be recommended. These episodes can become more frequent and severe over time.
- Infection or Inflammation
If a gall bladder stone causes infection (cholecystitis) or inflammation of the gall bladder, it becomes a medical emergency. In this case,
gall bladder stone surgery in Ahmedabad is often the only treatment option to prevent serious complications like gall bladder rupture.
- Obstruction of the Bile Duct
When a gall stone blocks the bile duct, it can lead to jaundice, pancreatitis, and other life-threatening conditions. Surgery is needed to remove the stone and restore proper bile flow.
- Chronic Digestive Problems
If gall bladder stones are causing frequent digestive problems, such as nausea, bloating, or indigestion, it may be time to consider surgery for better long-term relief.
- Risk of Gall Bladder Cancer
Although rare, untreated gall bladder stones may increase the risk of gall bladder cancer. In cases of chronic inflammation or symptoms that do not resolve, surgery may be necessary as a preventive measure.
Types of Gall Bladder Stone Surgery
There are two primary types of surgeries for gall bladder stone removal:
- Laparoscopic Cholecystectomy (Minimally Invasive)
This is the most common method used for
gall bladder stone surgery in Ahmedabad. It involves making small incisions in the abdomen, through which a camera and surgical tools are inserted. The gall bladder is then removed using these instruments. This method offers several advantages:
- Smaller incisions and faster recovery time
- Less pain after the procedure
- Shorter hospital stay
- Open Cholecystectomy (Traditional Surgery)
In some cases, especially if there are complications or if the gall bladder is severely inflamed, a traditional open surgery may be necessary. This involves a larger incision and a longer recovery period.
At
Dr Gastro, our surgeons are experienced in both procedures, using the most appropriate method depending on the severity of the condition.
What to Expect After Gall Bladder Stone Surgery
After your surgery, recovery time will vary depending on the type of surgery performed:
- Laparoscopic Surgery: Most patients can go home the same day or the next day. The recovery period typically lasts 1–2 weeks, and you can resume light activities shortly after.
- Open Surgery: Recovery may take 4–6 weeks, as the procedure is more invasive. Hospital stays are longer, and you will need to avoid strenuous activities during this period.
Aftercare Tips:
- Avoid fatty foods for a few weeks to allow your digestive system to adjust.
- Stay hydrated and eat light, easy-to-digest meals initially.
- Follow up with your surgeon for post-surgery checkups and monitoring.
Why Choose Dr Gastro for Gall Bladder Stone Surgery in Ahmedabad?

At
Dr Gastro, we offer the latest techniques for
gall bladder stone surgery in Ahmedabad. Our team of expert gastroenterologists and surgeons provide personalized care, ensuring the best possible outcome for each patient.
- Experienced Surgeons: Our surgeons are highly skilled in both laparoscopic and open surgery techniques.
- State-of-the-art Facilities: We use advanced diagnostic tools and modern surgical equipment.
- Comprehensive Care: From diagnosis to post-surgery recovery, we offer a full spectrum of care tailored to your needs.
Conclusion: Take the First Step Toward Relief
If you are experiencing symptoms of gall bladder stones, it’s essential to get a professional opinion.
Gall bladder stone surgery in Ahmedabad can provide lasting relief and prevent serious complications.
Schedule a consultation today at
Dr Gastro and take the first step toward a healthier, pain-free life. We are here to provide expert care for your gall bladder health.











 When Is the Right Time for Gall Bladder Stone Surgery?
The decision to have gall bladder stone surgery depends on several factors. Here are the key signs that surgery may be necessary:
When Is the Right Time for Gall Bladder Stone Surgery?
The decision to have gall bladder stone surgery depends on several factors. Here are the key signs that surgery may be necessary:
 At Dr Gastro, we offer the latest techniques for gall bladder stone surgery in Ahmedabad. Our team of expert gastroenterologists and surgeons provide personalized care, ensuring the best possible outcome for each patient.
At Dr Gastro, we offer the latest techniques for gall bladder stone surgery in Ahmedabad. Our team of expert gastroenterologists and surgeons provide personalized care, ensuring the best possible outcome for each patient.





 IMPORTANCE OF PROMPT ACTION
IMPORTANCE OF PROMPT ACTION
 WHAT TO EXPECT AFTER THE SURGERY?
WHAT TO EXPECT AFTER THE SURGERY?